Pelvic Floor Physiotherapy in Victoria
Continence and Pelvic Floor Dysfunctions are extremely common for Canadians. One in three women who have had children will develop urinary incontinence, and a woman’s risk of developing prolapse is two-fold after the first baby, and increases with subsequent pregnancies.
There are other conditions as well as pregnancy and childbirth that can contribute to the symptoms of pelvic floor dysfunction. These include prostrate surgery, menopause, aging, high impact exercise, poor bowel patterns and respiratory conditions are just a few of the many risk factors for developing symptoms. Pelvic Floor Dysfunction can have a huge impact on both a man and woman’s well being and quality of life.
Our full time Victoria Physiotherapists Holly Mallari, Shannon Huff & Leah Taylor have extensive experience and post graduate training in continence and pelvic floor physiotherapy and are committed to help prevent and manage the symptoms of pelvic floor dysfunctions. Our pelvic floor physiotherapy services are underpinned by a strong evidence research base. The current body of high level research has recommended pelvic floor exercises and treatment as a first-line treatment for many conditions.
Do you….
- Lose urine when you cough, sneeze, laugh or lift?
- Lose urine when you exercise?
- Know where every bathroom is at your local shopping mall?
- Lose urine when trying to unlock the door?
- Have to rush to the bathroom more than 8 times a day?
- Lose urine when you hear water running?
- Cope with wet underwear or clothing?
- Wear pads for catching urine?
Incontinence is a problem experienced by one in four women of all ages and lifestyles.
Many women have a problem with this after having a baby, as the growing weight of the baby and uterus can weaken your pelvic floor muscles. Pelvic floor muscles may also be injured during delivery. If left untreated, incontinence can worsen as you get older. Most incontinence can be significantly improved or cured without the need for medications or surgery.
 Pelvic Floor Physiotherapy can help in the following ways:
Pelvic Floor Physiotherapy can help in the following ways:
- We can determine the cause of incontinence and assess what treatment would be best for you.
- We can help you to strengthen your pelvic muscles using exercises and biofeedback.
- We can help you establish healthy bladder habits and assess your diet to ensure it is not contributing to your incontinence.
Please contact us for more information or to set up an appointment.
Pelvic Floor Physiotherapy and Pregnancy
A number of issues associated with pregnancy, labour, and delivery can be prevented and managed by Physiotherapy treatment. In addition to being fully qualified to assess and treat musculoskeletal issues, a Pelvic Floor Physiotherapist is trained to assess and treat pelvic floor dysfunction. Dysfunction of the pelvic floor can lead to pain, incontinence, pelvic organ prolapse, sexual dysfunction, inability to maintain activity levels, and decreased quality of life. Following is a description of problems common during pregnancy and an explanation of how Pelvic Floor Physiotherapy can help.
Pain During Pregnancy
Pain in the low back, pelvis, hip, and/or groin is common during and after pregnancy. There are three main reasons for this:
- 1. Your posture changes and your centre of gravity shifts as the baby grows, which results in greater stress being carried through the low back, pelvis, and hips.
- 2. The abdominal muscles stretch so much to accommodate the growing uterus that they can no longer adequately stabilize the low back and pelvis.
- 3. During pregnancy and breastfeeding, your body produces a hormone called relaxin to relax the joints of the pelvis and allow the baby to pass through the birth canal.
Unfortunately, relaxin affects all the joints in the body, which can contribute to pain in the areas described above.
In most cases these symptoms resolve within three months of delivery (or cessation of breastfeeding), but a qualified Physiotherapist can help to prevent, manage, and speed recovery from pain during pregnancy.
Blocked Breast Ducts
Blocked breast ducts can make nursing a challenge. A duct that remains blocked for a prolonged period is at risk of becoming infected. If you are concerned consult your doctor or public health nurse as soon as possible. If you have a fever you should see your doctor immediately.
If you have been referred for treatment for a blocked duct then you should be seen within 24 hours by one of our Women’s Health Physiotherapists experienced in this assessment and treatment. Our Physiotherapists are very supportive of any concerns that you may have regarding your breast feeding.
Treatment, if appropriate, usually consists of a specific dose of ultrasound to assist in the disruption of the blockage, soft tissue massage to move the blockage along the duct and heat. You will then be provided with a quiet area to nurse your baby. Education regarding what you can do at home will be provided.
 Incontinence
Incontinence
Urinary incontinence (the inability to control the flow of urine) is common during pregnancy and after delivery. During pregnancy, the growing uterus pushes on the bladder and causes increased frequency of urination. If the pelvic floor muscles aren’t strong enough to resist the extra stress, incontinence may result.
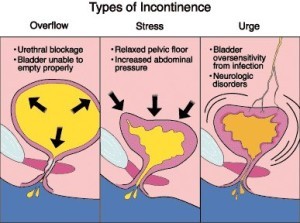
There are three main types of urinary incontinence:
1. Stress urinary incontinence: leaking of urine with strenuous movements and activities (ex. coughing, sneezing, laughing, jumping, squatting)
2. Urge urinary incontinence: leaking of urine associated with a strong uncontrollable urge to void
3. Overflow incontinence: bladder is unable to empty properly due to urethral blockage.
Pelvic Organ Prolapse
Pelvic organ prolapse is the descent of one or more of the female pelvic organs (bladder, uterus, and/or rectum) into or through the vagina. The pelvic floor muscles, organs, and ligaments can be stretched or damaged during pregnancy, labour, and delivery. Without proper management, this can lead to pelvic organ prolapse. Symptoms of pelvic organ prolapse include a feeling or pressure or fullness in the lower abdomen, low back or pelvic pain, dyspareunia (pain with intercourse), incontinence, and bowel problems such as constipation.
Women who continue to have symptoms of incontinence more than three months after delivery have a significantly increased risk of recurrent incontinence and pelvic organ prolapse later in life. Pelvic Floor Physiotherapy treatment, which includes manual therapy, education, lifestyle modification, and exercise prescription, can prevent and treat incontinence and pelvic organ prolapse in women after childbirth.
Exercise During and After Pregnancy
Many women continue to be very physically active during pregnancy. In most cases, women can continue to exercise throughout pregnancy, albeit with some modification as time goes on. A Physiotherapist can provide education, specific exercises, and appropriate bracing to allow you to be physically active throughout your pregnancy. It can also be difficult to return to pre-pregnancy activity levels after labour and delivery. A Physiotherapist can assess muscle activation, biomechanics, and core stability to ensure an appropriate, safe, and timely return to exercise. Exercise and Pregnancy Fact Sheet.
Our Victoria Pelvic Health Physiotherapist Team

- Registered Physiotherapist
- Functional Dry Needling/IMS
- Special Interest in Shockwave Therapy
- Pelvic Floor Physiotherapist
- Special Interest in Pregnancy Related Pelvic Floor Issues
- EMG Biofeedback
- Pre and Postnatal Pelvic Health
- Special Interest in Track & Field/Running Injuries
- Kinesiologist
- ICBC Approved Physiotherapy Provider
Holly Mallari is a Pelvic Floor Physiotherapists practicing at
Shelbourne Physiotherapy (Downtown Cook Street Clinic) at #308–1175 Cook St., Victoria, BC, V8V 4A1 and our main Clinic located at 100B-3200 Shelbourne Street.
For more information on their education, background, and treatment approach, please click on their names to see their biographies;
To book an appointment with Shannon Huff or Leah Taylor call 250-598-9828 or Holly Mallari please call (250) 381-9828.
What is your Pelvic Floor?
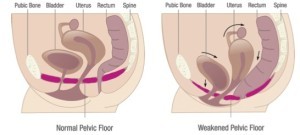
The pelvic floor is a group of muscles and ligaments which support the bladder, uterus (womb) and bowel. The openings from these organs, the urethra from the bladder, the vagina from the uterus and the anus from the bowel pass through the pelvic floor. The pelvic floor muscles attach to your pubic bone at the front and the tail bone at the back and from the base of your pelvis.
The pelvic floor is the base of the group of muscles referred to as your ‘core’. These muscles are located in your pelvis, and stretch like a trampoline or hammock from the pubic bone (at the front) to the coccyx or tail-bone (at the back) and from side to side. The pelvic floor muscles work with your deep abdominal (tummy) and deep back muscles and diaphragm to stabilize and support your spine. They also help control the pressure inside your abdomen to deal with the pushing down force when you lift or strain – such as during exercise. Pelvic floor muscles support the bladder and bowel in men, and the bladder, bowel and uterus in women. They also help maintain bladder and bowel control and play an important role in sexual sensation and function.
What do the pelvic floor muscles do?
When the pelvic floor is strong, it supports the pelvic organs to prevent problems such as:
- incontinence (the involuntary loss of urine or feces)
- prolapse (lack of support) of the bladder, uterus and bowel.
The pelvic floor muscles also help you to control bladder and bowel function, such as allowing you to ‘hold on’ until an appropriate time and place.
What causes pelvic floor muscle weakness?
Some of the common causes of pelvic floor muscle weakness are:
- childbirth – particularly following delivery of a large baby or prolonged pushing during delivery
- being overweight
- constipation (excessive straining to empty your bowel)
- persistent heavy lifting
- excessive coughing – causing repetitive straining
- changes in hormonal levels at menopause
- growing older.
How do I strengthen my pelvic floor muscles?
It is recommended that all women exercise their pelvic floor muscles everyday throughout life, to prevent weakness or improve strength. Exercising weak muscles regularly, over a period of time can strengthen them and make them work effectively again. Regular gentle exercise, such as walking can also help to strengthen your pelvic floor muscles.
Exercise 1 (long hold for strength)
Step 1:
Sit, stand tall, lie on your back with your knees bent and legs comfortably apart or kneel on your hands and knees.
Step 2:
Close your eyes, imagine what muscles you would tighten to stop yourself from passing wind or to ‘hold on’ from passing urine. If you can’t feel a distinct tightening of these muscles, ask for some help from a women’s health physiotherapist. She will help you to get started.
Step 3:
Now that you can feel your pelvic floor muscles working, tighten them around your front passage, vagina and back passage as strongly as possible and hold for three to five seconds. By doing this, you should feel your pelvic floor muscles ‘lift up’ inside you and feel a definite ‘let go’ as the muscles relax. If you can hold longer (but no more than a maximum of eight seconds), then do so. Remember, the squeeze must stay strong and you should feel a definite ‘let go’. Repeat up to ten times or until you feel your pelvic floor muscles fatigue. Rest for a few seconds in between each squeeze.
Steps one to three count as one exercise set. If you can, do three sets per day in different positions. Do your pelvic floor exercises everyday for the rest of your life.
Exercise 2 (quick squeeze for power)
Squeeze and lift your pelvic floor muscles as strongly and as quickly as possible. Do not try to hold on to the contraction, just squeeze and let go. Rest for a few seconds in between each squeeze. Repeat this 10 to 20 times or until you feel your pelvic floor muscles fatigue.
If you can, do this exercise set one to three times per day.
During both exercises you should:
- feel your pelvic floor muscles ‘lift up’ inside you, rather than feel a downward movement
- relax your thighs and buttocks
- keep breathing normally
- stop exercising if your muscles fatigue.
What can I do to prevent damage?
To prevent damage to your pelvic floor muscles, avoid:
- constipation and/or straining with a bowel motion
- persistent heavy lifting
- repetitive coughing and straining
- putting on too much weight.
Make training part of your life by:
- tightening your pelvic floor muscles every time you cough, sneeze or lift
- doing some regular exercise, such as walking
- progressing your exercises by doing them during the day in different positions e.g. standing, sitting or on your hands and knees.
Shelbourne Physiotherapy offers the Pilates Pelvic floor conditioning program to improve pelvic floor weakness and improve the symptoms of incontinence.
Holly Mallari Incontinence Physiotherapist Shelbourne Physiotherapy-Cook Street Victoria Clinic
Victoria,
British Columbia
V8V 4A1
CA
Phone: 250-381-9828
Website: https://physiotherapyvictoria.ca

